The Traffic Jam In The Nose
Why is my nose always blocked… and why can’t I smell anything?
Many patients come to see me for “sinus problems.”
But not the usual allergic rhinitis — the sneezing, the runny nose.
This is different.
This is:
A nose so blocked…
it feels like a Friday evening traffic jam on Federal Highway.
No airflow.
No relief.
No matter what you try.
And most of the time?
These patients have already:
Seen multiple ENT specialists
Tried multiple medications
Some have even had surgery
And yet… it keeps coming back.
The Questions That Change Everything
When I meet these patients, I ask a few very specific questions:
- “Did your surgeon mention polyps during your scope or surgery?”
- “Can you still smell?”
- “Do you react to aspirin or painkillers?”
- “Do you have asthma?”
And patients often ask me:
“Why all these questions?”
What’s Really Going On?
This condition is called:
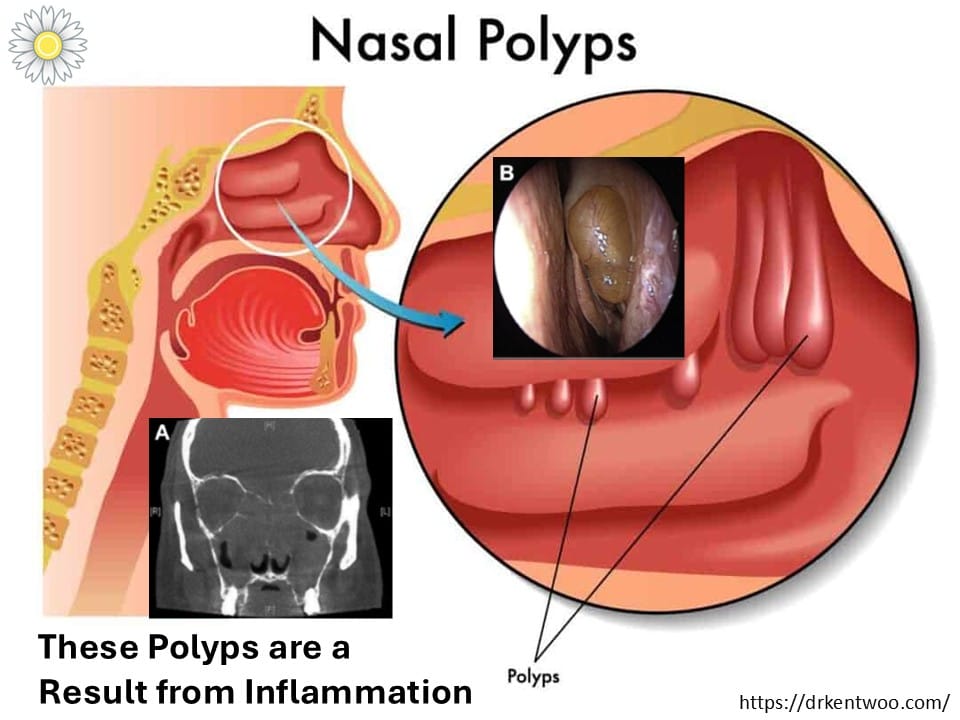
👉 Chronic Rhinosinusitis with Nasal Polyps (CRSwNP)
Let’s simplify it.
- Chronic → long-standing
- Rhinosinusitis → inflammation of the nose and sinuses
- Polyps → soft, grape-like swellings inside the nose
They’re not cancer.
But they are space-occupying troublemakers.
They grow slowly…
Block airflow…
Trap mucus…
And affect your sense of smell.
Why Your Nose Feels Permanently Blocked
Think of your nose like a room.
Now imagine:
- The walls are swollen
- The windows are blocked
- And someone keeps placing soft balloons inside
That’s what polyps do.
So even with sprays or medication…
👉 There’s simply no space left for air to flow.
The Smell Clue
One of the biggest clues?
👉 Loss of smell
If you tell me:
“Doctor, I can’t smell my food anymore…”
That immediately raises a flag.
Because in this condition, smell loss is not just blockage —
it’s also inflammation affecting the smell receptors.
The Asthma & Painkiller Link
Some patients will also say:
- “Yes, I have asthma.”
- “Yes, certain painkillers make me worse.”
This combination matters.
It may point to a pattern called:
👉 Aspirin-Exacerbated Respiratory Disease (AERD)
Which includes:
- Nasal polyps
- Asthma
- Sensitivity to aspirin/NSAIDs
So this is not just a nose issue.
👉 It’s a whole airway condition.
Why It Keeps Coming Back
This is where frustration builds.
You’ve tried medication.
Maybe even surgery.
But the polyps return.
Why?
Because surgery removes the polyps…
but not the underlying inflammation.
It’s like:
Mopping the floor…
while the tap is still running.
So What Actually Helps?
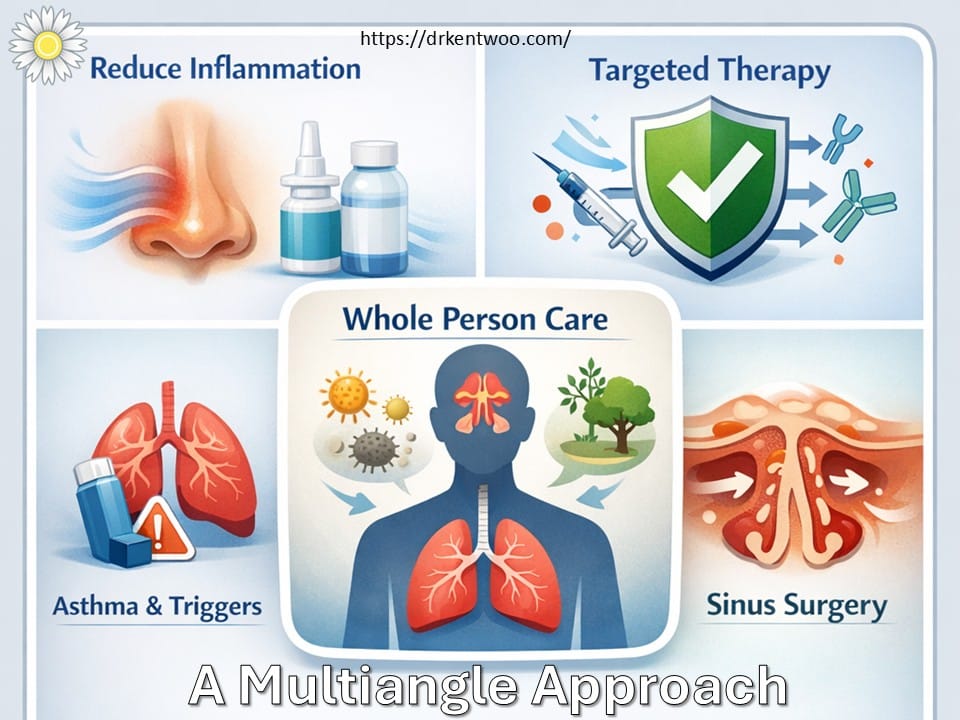
This condition is about control — not quick fixes.
We approach it from multiple angles.
1. Reduce inflammation
- Nasal steroid sprays or rinses
- Short courses of oral steroids (when needed)
2. Control the immune response
- For more severe cases → biologics (targeted therapies)
3. Look at the bigger picture (this is important)
Traditionally, this condition was thought to be non-allergic.
But newer studies are showing something interesting.
👉 There can be overlap.
Some patients with nasal polyps also have:
- Underlying allergic triggers
- Ongoing environmental exposures
- Immune patterns that behave like allergy-driven disease
And this matters.
Because as an allergist, I don’t just treat the polyps.
I treat you as a whole.
So part of the plan may include:
- Identifying allergy contributions
- Reducing exposures
- And in selected cases → allergen immunotherapy
Not for everyone.
But for the right patient, it can make a meaningful difference.
4. Treat associated conditions
- Asthma control
- Avoiding trigger medications (like certain painkillers)
5. Surgery (when needed)
- To clear blockage
- But always combined with long-term medical control
The Key Shift
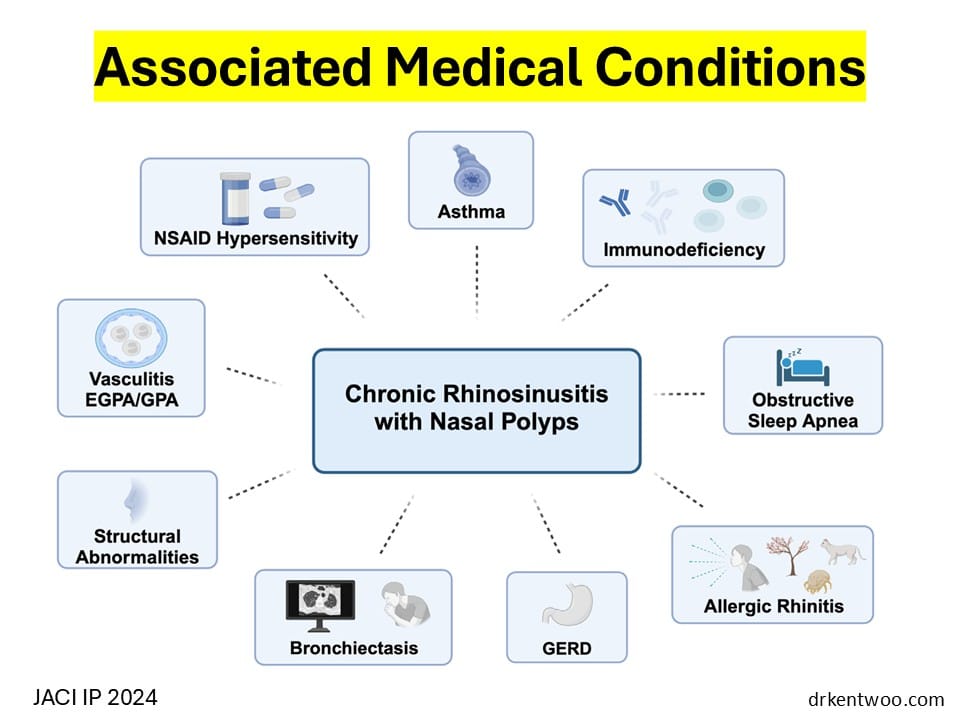
This is what I want patients to understand:
This is not just a sinus problem.
This is an immune system problem showing up in your nose.
Once you see it that way…
The repeated cycles start to make sense.
A Final Thought
If you’ve been:
- Constantly blocked
- Unable to smell
- Going through repeated treatments or surgeries
You’re not imagining it.
And you’re not “failing treatment.”
You’ve just been dealing with a condition that
needs a different strategy.
Let’s Figure It Out Together
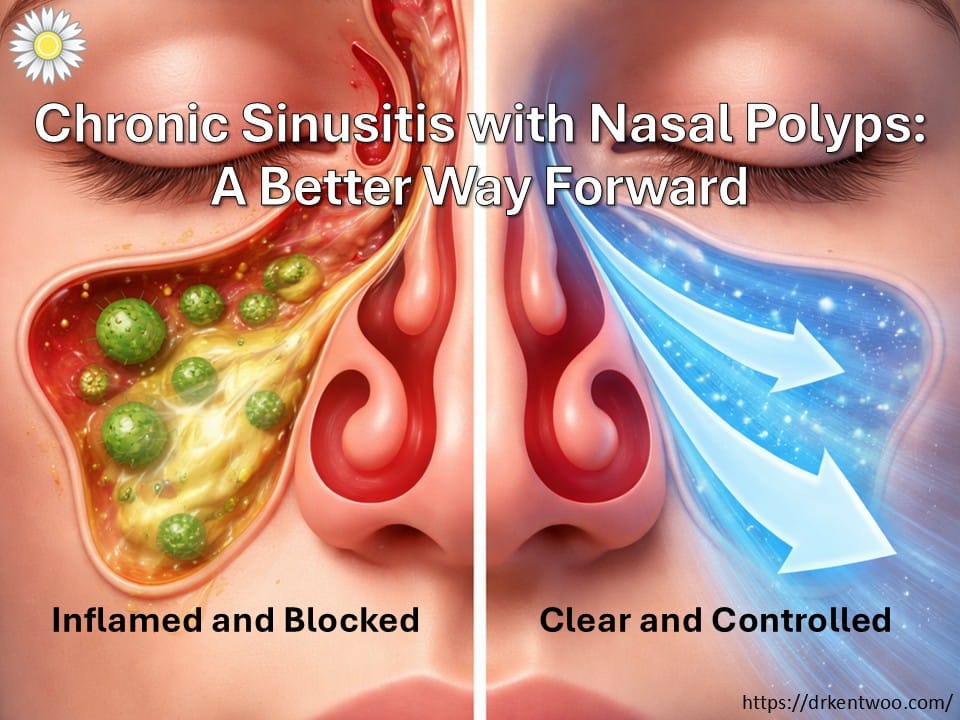
Sometimes, what patients need is not just another medication.
They need:
- A clearer explanation
- A proper plan
- And someone to connect the dots
If this sounds like your story,
bring it up during your visit.
We’ll go through it step by step.
Because once you understand the problem…
you can finally start taking control of it.