Stress and Urticaria: When Hives Flare Under Pressure

She had seen several doctors before coming to see me.
Her hives were controlled with medication.
They would settle.
Then they would return.
As we spoke, I noticed her shoulders were tense. Her breathing shallow.
I asked, “What do you do for fun?”
She paused.
“Fun? I have too much work.”
“Is work stressing you?”
She looked surprised.
“Yes. How did you know?”
The Mind–Immune Connection
Stress does not “cause” urticaria the way allergies can.
But stress can lower the threshold for flares.
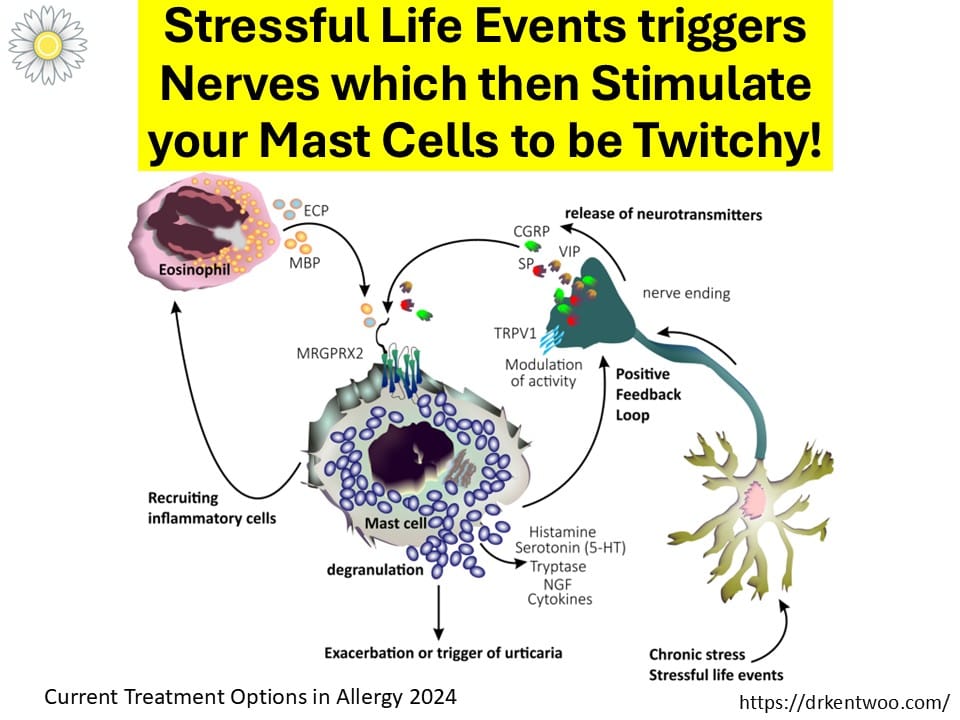
When you are under ongoing stress, your nervous system releases chemicals that make mast cells — the cells that release histamine — more reactive.
More reactive mast cells mean:
- More histamine
- More itch
- More swelling
- More hives
Stress does not mean the hives are imaginary.
It means your immune system is listening to your nervous system.
Why It Keeps Coming Back
Many patients say:
“It improves with medicine, then it returns.”
Medication blocks histamine.
But if stress levels remain high, mast cells remain sensitive.
The cycle can look like this:
Stress → Hives → More stress → More hives
Breaking the cycle means addressing both the immune response and the stress response.
Five Things That Actually Help

These are simple.
But consistency matters.
1. Breathe slowly for 3–5 minutes daily.
Slow diaphragmatic breathing calms your stress response.
2. Move gently every day.
A 20–30 minute walk or light yoga reduces stress hormones and improves sleep.
3. Protect your sleep.
Reduce late-night screens. Sleep stabilizes immune balance.
4. Cut back on stimulants during flares.
Caffeine and alcohol can worsen itch and anxiety.
5. Have a clear action plan.
Work with your doctor on antihistamine timing and flare management.
When you have a plan, uncertainty reduces.
And uncertainty itself is stressful.
When Stress Feels Bigger Than Skin

Some patients hesitate to talk about stress.
There is still stigma around seeing a therapist or psychologist.
We do not replace mental health professionals.
But sometimes, patients simply want to talk in a safe clinical space.
We understand that.
If you feel that stress is driving your flares, we can:
- Schedule more frequent follow-ups
- Help you structure a flare-response plan
- Provide a consistent point of contact
- Discuss lifestyle adjustments
- Introduce our wellness support options
For some patients, knowing there is a steady place to return to reduces anxiety.
And when anxiety reduces, the skin often follows.
We also offer structured wellness programs for patients who need time to reset and step away from ongoing stressors.
But we will not know unless you tell us.
A Reassuring Perspective
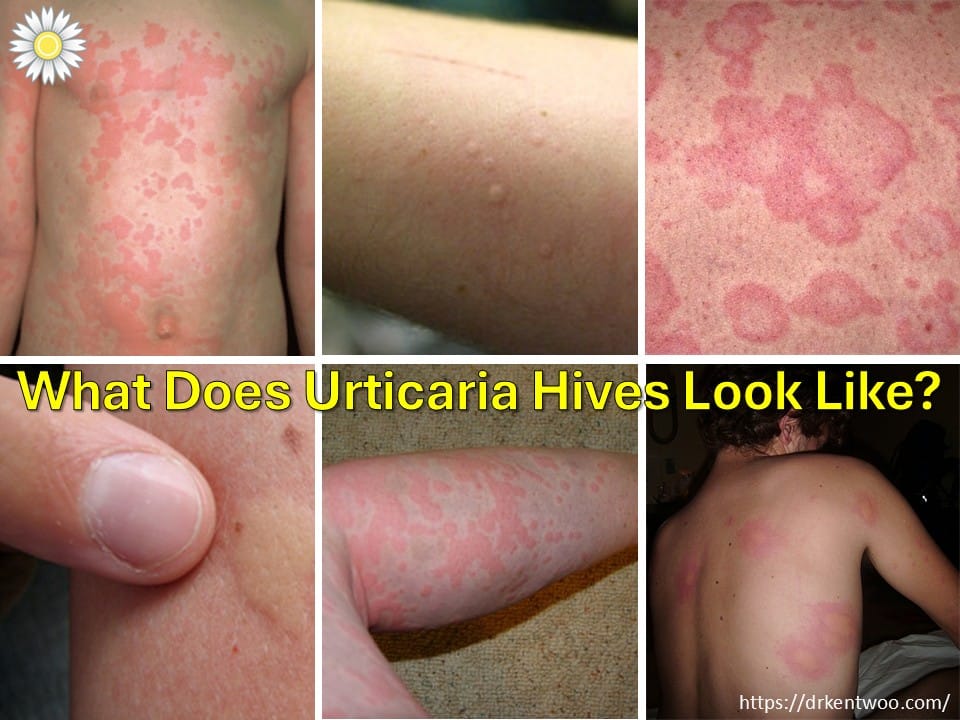
Chronic urticaria is common.
Yes it is distressing!
But it can be treated
Medication is important.
But calming the nervous system is part of care too.
Managing hives is not just about blocking histamine.
It is about lowering the overall reactivity of the body.
If stress is playing a role, speak about it openly.
Your skin may be asking for more than just another tablet.
Continuity.
Clarity.
Steady care.
🔎 Learn more: [Chronic Urticaria and Autoimmune Links]